Author/Blogger Reggie Simpson
-
06 Dec, 2015
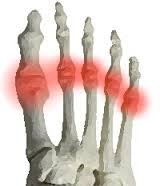
A High Risk Foot Issue
If you’ve been suffering with the joints in your feet, these may be indicative of a more serious underlying issue, such as Rheumatoid Arthritis.
What is Rheumatoid Arthritis?
Rheumatoid Arthritis is a condition that results in your body’s immune system weakening and turning on itself. As a result, your immune system will produce substances that attack your joints rather than protect them, resulting in inflammation, discomfort and pain.
The symptoms of Rheumatoid Arthritis may include joint pain, general stiffness, swelling, tiredness, fever, loss of appetite and/or sudden weight loss.
What are the known causes of the condition?
While the exact cause of Rheumatoid Arthritis is currently unknown, there are a number of factors that place certain individuals at higher risk of developing the condition.
Some may find that they are genetically more likely to experience it throughout their lifetime while others have developed it after exposure to certain chemical or environmental triggers.
What makes Rheumatoid Arthritis a high-risk issue?
There are several risk factors that can lead to the development of Rheumatoid Arthritis - as well as being genetic in many cases, so it’s important to take notice of these and keep track of your joints to catch the condition developing in its early stages.
Factors include:
• Gender. Women are more likely to develop the condition.
• Age. It occurs mostly in those aged 40 – 60.
• Family history.
• Poor environmental factors. By living an unhealthy lifestyle, you are at higher risk of developing health conditions as a whole, including RA.
What preventative measures can be taken to lower the risk of developing Rheumatoid Arthritis?
There are currently no preventative measures that can be taken to directly prevent Rheumatoid Arthritis; it is worth considering the risk factors involved.
While some people may be genetically predetermined to develop Rheumatoid Arthritis, others may find that simple lifestyle changes can lessen the risk of developing the condition.
Smoking, for example, is a known risk factor, so that’s yet another reason to try giving up if you haven’t already.
How can people who already have the condition properly deal with the effects?
There is no cure for Rheumatoid Arthritis; however, there are things sufferers can do to make the impact of the disease more manageable.
By getting support from health professionals, medication, supportive treatments or surgery, it is possible to reduce inflammation and significantly alleviate pain, slow damage to the joints, improve mobility and enable you to live a healthy lifestyle.
If you are at risk of developing Rheumatoid Arthritis or have noticed any changes in your feet that may be a sign of the condition, it’s important to pay your podiatrist a visit as soon as possible for an evaluation. They’ll be able to suggest the best method of treatment and ongoing care to ensure your health and comfort.
Contact Betafeet Podiatry today to book your appointment and take a step towards healthier joints.