29 Nov, 2016
By Matthew Collison
New Foot Screening App
Foot problems related to diabetes are common, and sensation and the blood supply to the feet can be impaired, which if not detected early enough can predispose a patient to ulceration and in some cases amputation. There are over 7000 diabetes related amputations annually in England, and many of these are preventable. Early detection of foot problems in patients with diabetes is vital in preventing these, including an annual foot check and ongoing monitoring and management by a podiatrist and the wider medical team as required. One of the most important issues however, is an individual’s awareness of their own condition and how it affects their feet.
Over the past year, I have been fortunate to be involved in a project with our professional body, the College of Podiatry and Foot in Diabetes UK as well as other professional groups including the Royal College of Physicians and Surgeons of Glasgow, the British Association of Prosthetists and Orthotists on the development of a smartphone and tablet app for patients with diabetes on maintaining their foot health. The app is also recognised by the Royal College of Nursing and Diabetes UK.
- For people with diabetes, this App has been developed through a unique multi-disciplinary collaboration, based on nationally approved guidelines. Supported by videos, this app and provide the following:Advice and information on your condition, exploring how diabetes can affect your feet
- Track your routine screening appointments and offer reminders when they are due/upcoming
- Detailed, practical information on how to look after your feet in accordance with nationally recognised and agreed guidelines and how to recognise when to seek advice.
I would encourage all of our patients with diabetes (or family members) to download the free app to their devices, as it provides straightforward, practical advice on looking after your feet, and how to recognise when things go wrong (and when and how to seek help).
The app is available on Apple iOS and will be available on Android devices soon. For more information, search for diabetic foot screening app on the app store, or visit:
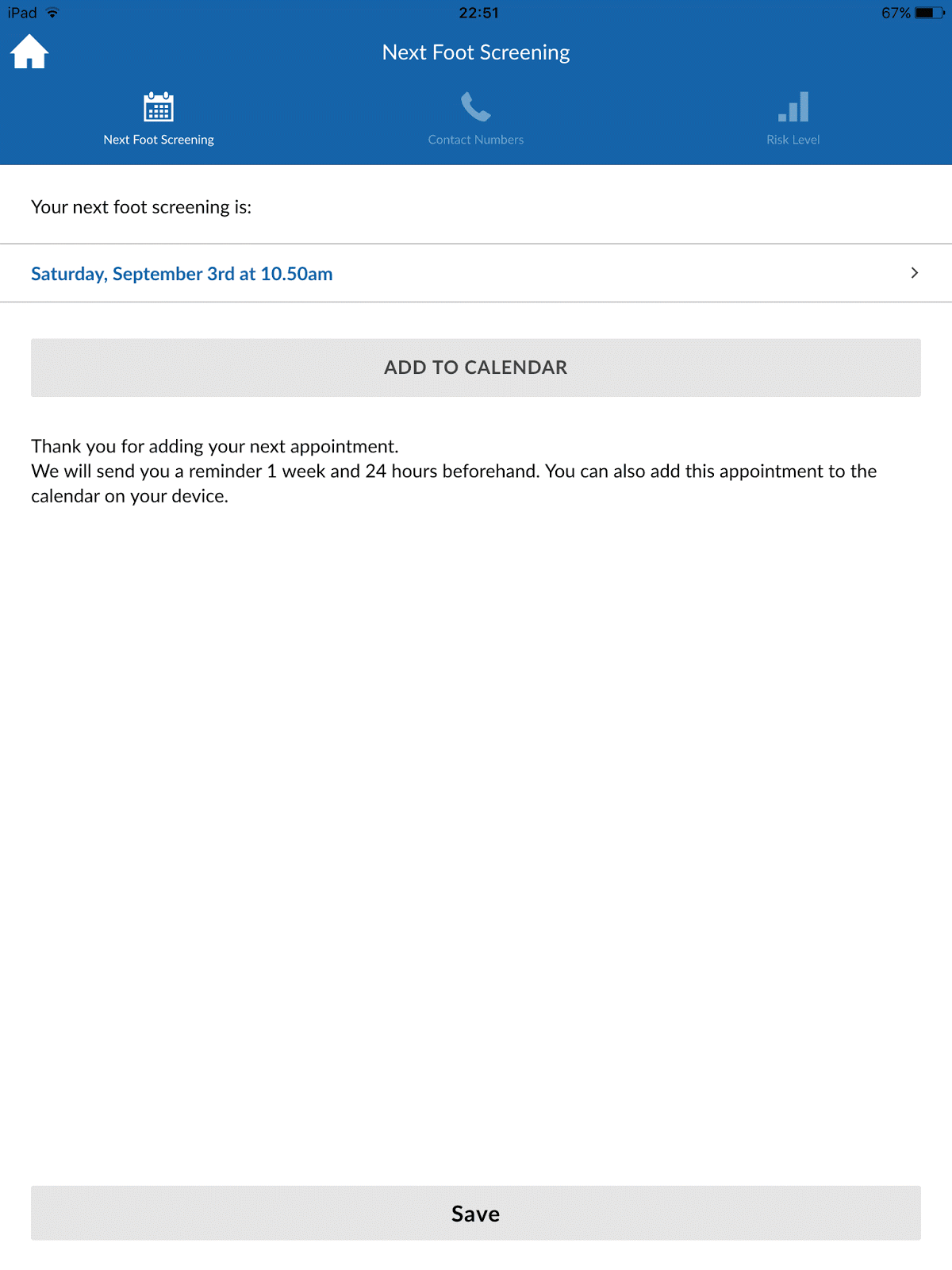
Pics 1 and 2 (below): The app includes videos on what to expect at your annual foot assessment and
allows you to save your appointments to your calendar and it notifies you beforehand. It also allows you to store important numbers including your GP, podiatrist and hospital foot clinic.