08 Jan, 2017
Author/blogger Reggie Simpson with thanks to the Society of Chiropodists and Podiatrists and NHS Choices
What are they and how do you treat them?
Season’s Greetings from my birthplace of Ohio (yes, one of the defining US swing states for Donald Trump! ).
I managed to miss out on the heavy snow and sub-freezing temperatures (-24C at their lowest). Temperatures then rose briefly to 15C and then returned to the average norm (-1C to 6C). With the Lake Erie effect, the wind chill makes it even colder. Potential chilblain weather .
What are they?
For those who like to study the etymology of words, ‘chilblain’ comes from the Old English ‘cele’ – chill/cold + blain/‘blegen’ – a sore. The modern medical definition of chilblain is pernio or perniosis, and is a localised form of vasculitis.
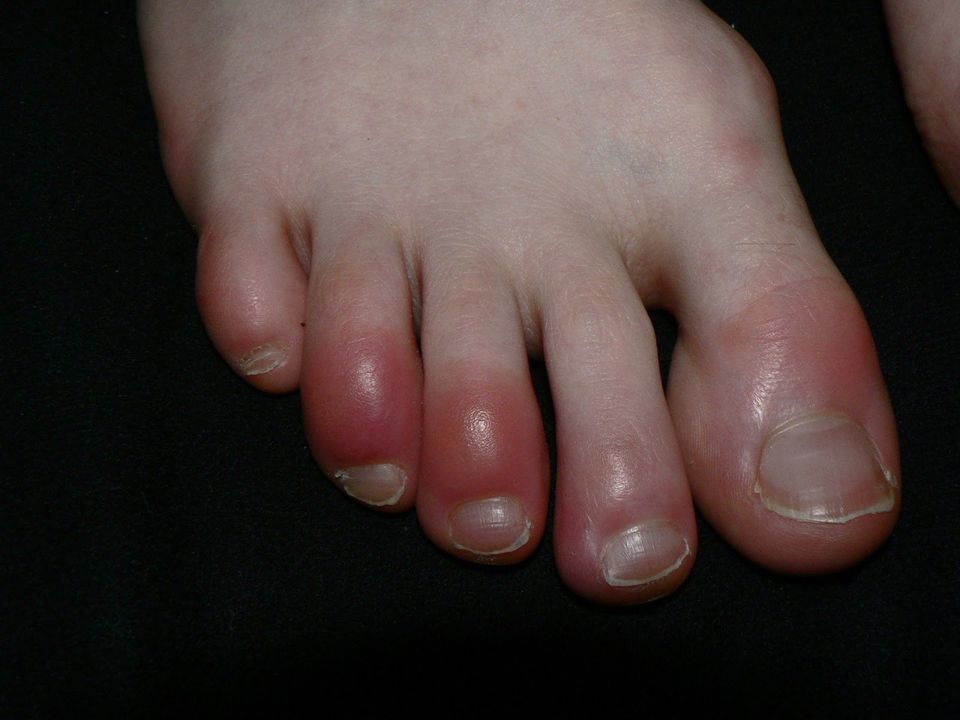
Chilblains are small, itchy, red (and sometimes purple) swellings on the skin, which can become increasingly painful. They usually develop several hours after exposure to the cold. They typically cause a burning and itching sensation and when they dry out they can cause cracks in the skin. It is important not to scratch the skin as it can break easily and become infected.
Chilblains most often occur in the toes, fingers, the face (particularly the nose) and the earlobes. They can also occur in areas exposed to pressure, such as bunions.
Chilblains should not be confused with frostbite. Frostbite is an injury to the body that is caused by freezing and exposure of the body to cold temperatures for a prolonged period of time. Frostbite can permanently damage the body, and in severe cases can lead to amputation. Those who have reduced blood circulation and those who don’t dress properly for the extremely cold temperatures face increased risk of frostbite.
Although chilblains are most associated with cold weather, damp conditions can also bring about chilblains. The condition can also be worsened by poor circulation, often diabetics and the elderly people have poor circulation and prone to peripheral vascular disease, low body weight, poor nutrition or health, lack of exercise, hormonal changes, genetics and family history. Also those who have connective tissue disease such as lupus erythematosus, anemia, Raynaud phenomenon, systemic sclerosis may be more prone to chilblains. Those who smoke are more at risk of chilblains as nicotine constricts blood vessels.
How do chilblains develop?
Chilblains develop when tiny blood vessels under the skin constrict because of any or all of the aforementioned conditions, reducing the flow of blood until the area warms up and causes some leakage into surrounding tissues. You may remember how exposure to cold weather makes your skin tingle as it warms up, but this does not necessarily mean you have chilblains.
How do you prevent them?
The best advice is prevention, and chilblains can be prevented by keeping your legs, feet, and body warm, especially if you have poor circulation and your mobility is limited. Wear warm clothes, socks and gloves to keep to hands and feet warm which are not too tight, keep your whole body warm and if needed carry around a form of portable heater such as the G-Tech Hand Warmer – (a portable warming pouch offering instant heat anytime, anywhere). Warm up slowly when cold and do not use too hot direct heat. Exercise and move about don’t sit for too long so that the blood flow keeps pumping; especially before and during outdoor activities. Avoid medicines that might constrict blood vessels: this may be problematic with some blood pressure medication, please discuss alternatives with your GP, also known to constrict the blood vessels are caffeine, decongestants, diet aids and smoking.
How do you treat chilblains?
Chilblains often get better on their own without treatment after a week or two. However, there are various home remedies such as soothing lotions you can use such as witch hazel and calamine or speak to your pharmacist. If your chilblains continue to be a problem or have ulcerated, get advice from your podiatrist, who may refer you on to your GP for medical treatment. Equally, your GP may refer you to your podiatrist for specialist chilblain and related foot care. If your chilblains are severe and keep returning, your GP may recommend taking a daily dose of a medication called Nifedipine. This works to relax the blood vessels and improve circulation.
Other treatments may include:
Topical corticosteroid cream applied accurately for a few days to relieve itch and swelling.
Antiseptic dressings, antibiotic ointment or oral antibiotics for secondary infection if required.
You can read more about how to keep warm in very cold weather and looking after your health in the winter in the following links:
http://www.nhs.uk/Livewell/winterhealth/Pages/Verycoldweather.aspx
http://www.nhs.uk/Livewell/winterhealth/Pages/Winterhealthhome.aspx
Don’t suffer in silence! Visit Betafeet Podiatry today, conveniently located in Hemel Hempstead and Tring.