17 Feb, 2017
Author/blogger Reggie Simpson
Introducing new technology at Betafeet Podiatry
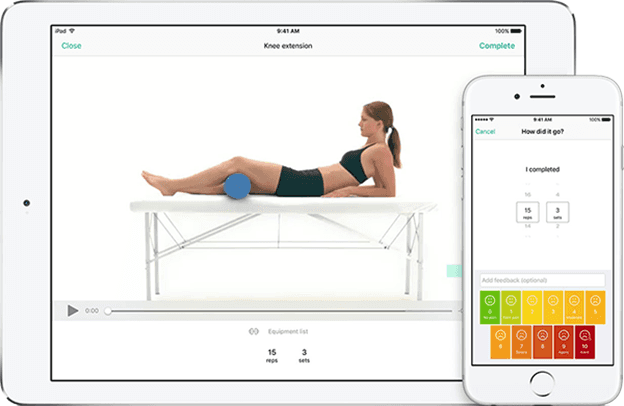
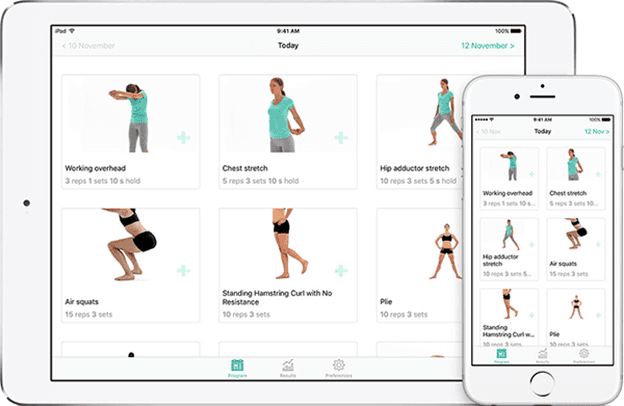
At Betafeet Podiatry we pride ourselves in offering our patients the latest technologies to help you achieve your outcomes. We are pleased to announce that we are offering a new treatment which will help to create tailored exercise programmes for you using a brand-new app called PhysiApp.
PhysiApp will let you complete your prescribed exercise programme by following crystal-clear, narrated exercise videos. The app is completely free to download from the App store and Google Play store or can be accessed via your web browser. Built-in reminders help you move forward to a better you!
Of course, there are other ways to get you 'on track' with exercises equally free and not reliant on mobile technology.
I, for one, have been exploring opportunities to participate in fitness outings and have joined in walks organised by Simply Walk (
) around College Lake Nature Reserve, Tring. I spotted their poster in a a local car park. I also recently picked up a leaflet from the Tring Silk Mill Community Centre entitled Hertfordshire Health Walks ( www.hertfordshirehealthwalks.org )
Contact Hertfordshire, Buckinghamshire and/or Bedfordshire county councils for more information on walks within the three counties and beyond; many of these are accessible by public transport and cater for varying ability levels, ages and interests. Your local library is also well worth a visit to help you get more information.
These are all great ways to get fitter and meet new people, whilst enjoying some fresh air, good company and beautiful countryside! Hats off to the myriad of volunteers who keep these walks 'going'.
Stay tuned for more information on the use and impact of Physitrack by Betafeet's own Matt Collison, who has been commissioned to write an article about PhysiTrack for Podiatry Now . In the meantime, do ask about whether you can benefit from the app at a future visit with us.