By Author/Blogger Reggie Simpson
01 Dec 2015
Caused by the Human Papilloma Virus (HPV)
You may have experienced a verruca at some point during your life, or maybe you currently have one you’re looking to remove. If so, perhaps you’re wondering what exactly it is, why it occurred and how they can be easily treated. Read on to learn more about the causes and treatments of verrucae and when to seek further advice.
What exactly is a verruca?
A verruca, sometimes referred to as a ‘plantar wart’, is a wart that develops on the body’s plantar surfaces – the soles of your feet. It is often the case that the pressure of walking or standing for long periods pushes the warts into the skin, causing painful bumps on the surface. They can appear either alone, or in a cluster – which are known as mosaic warts.
What are the symptoms of verrucae?
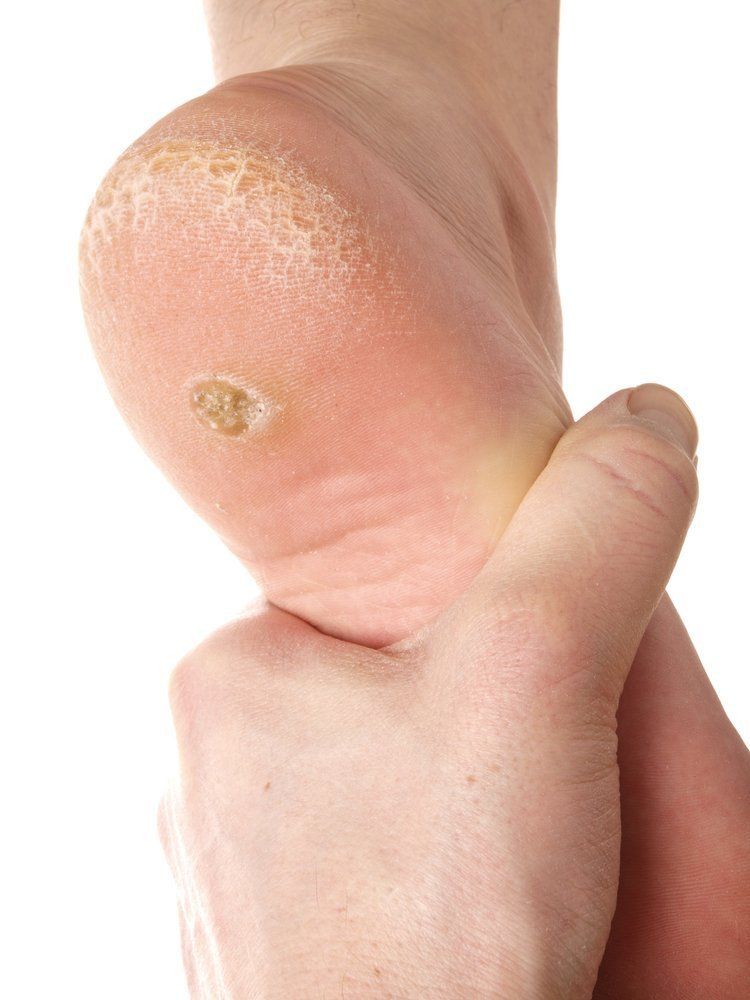
The symptoms of verrucae are easy to spot. You’ll notice a small growth on the foot, which will often have small black or darkened dots on its surface. You may also feel pain whilst putting pressure on your feet.
How can a verruca be treated?
The treatment you choose for your verrucae will depend on their severity, as well as your own personal pain tolerance.
Verrucae will usually go away on their own as a result of the body’s natural immune system, so if you find them to be unnoticeable, you may consider simply waiting it out.
However, if verrucae are affecting your day to day life, it’s important to sort them. There are a number of over the counter remedies available; however, there is no single miracle cure that will work every time, so a little trial and error is to be expected.
How can verrucae be prevented?
Prevention is simpler than the cure, so it’s worth taking the steps to avoid their development:
• Keep your feet protected when visiting communal changing rooms or pools.
• Don’t touch other peoples’ verrucae.
• Don’t share towels with people who have verrucae.
• Don’t pick at your verruca as you may encourage the virus to spread.
• Wear clean socks daily and keep your feet dry.
When should I seek the advice of a professional?
Verrucae are viral in nature, so in most cases, the body will take care of it on its own. However, if you’re continuing to experience verrucae on a regular basis, it’s possible to have them treated with cryosurgery or needling. A professional will also be able to take a look at underlying issues that have made verrucae unresponsive to your previous at-home treatments.
If you’ve tried over the counter solutions only to find them to be ineffective, it may be time to visit a professional for further evaluation and treatment.
If you’re concerned about verrucae or any other foot-related issue, a trained podiatrist can help. Get in touch with Betafeet Podiatry and book an appointment today to ensure your foot problems are diagnosed and treated in good time.