Get your feet sandal-ready for the summer!
Blog updated April 25 2018
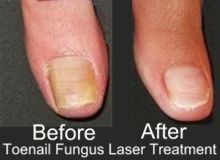
Do you suffer from fungal nail infections? Not only are they unsightly; they can also cause discomfort and pain.
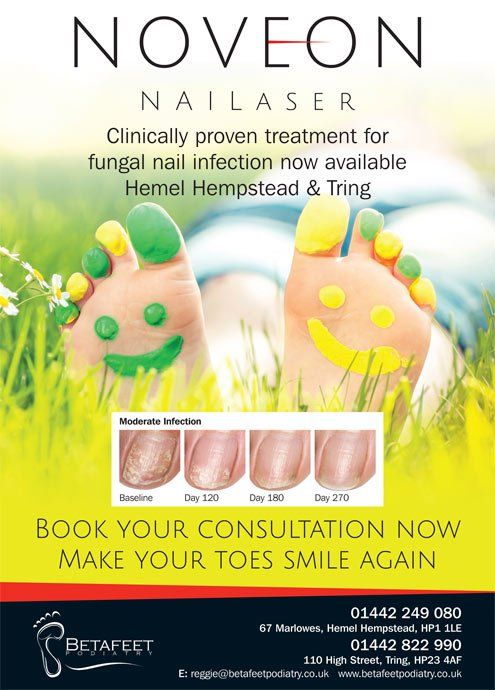
Our Hemel clinic offers Noveon®, a state of the art laser technology backed by research. And, for a limited time (May, June and July 2018), we are offering the treatment for a reduced price of £400 for up to four treatments and up to four nails, saving you £200 off the normal price. You will, of course, need to have a pre-treatment assessment appointment (£50) before you begin your treatment sessions. Your podiatrist will review the areas you want/need to be treated, ensuring you are suitable for this treatment and answer any questions you might have.
How does it work?
Fungus, bacteria and yeast are prime causes of fungal nail. Yeasts and moulds combine with dampness to cause toenail fungus. Wearing tight-fitting shoes or not letting feet dry out gives toenail fungus a place to grow. Other risk factors include diabetes, a compromised immune system, or an abnormal PH skin level. The likelihood of toenail fungus increases with age, which leads to reduced blood circulation and more risk of exposure.
Noveon® is the safest and most effective treatment option available. The laser is able to kill the fungus using certain light wavelengths that are known to disrupt the metabolism of fungal cells. Once their metabolism has been altered, the fungal cells die. Meanwhile, healthy skin and tissue cells are left unharmed.
The laser works by targeting the infected nail or nails with two unique wavelengths of laser light. Whereas other laser treatments for fungal nails do so at high temperatures (which often cause pain or discomfort during treatment), Noveon® treats at lower temperature levels.
Noveon® treatment also reduces fumes (plumes) which can affect both patient and user. Laser plume may contain carcinogens, irritants and fine dusts. Plumes may also contain viruses and cancer cells, blood fragments, and bacteria spores. They also contain carbon monoxide, hydrocarbons, and various toxic gases. Plumes may contain chemicals such as formaldehyde, hydrogen cyanide, and benzene.
What can I expect with this treatment?
A session involves having the affected toe or toes being hooked up to the Noveon® laser machine. A typical treatment consists of three/four 16-minute treatments, in all around 120 days.
But first there will be an initial consultation 10-14 days before starting your first treatment. This will involve:
·Signing a consent form and receiving information on the treatment
·Pre-treatment
·Q & As
·Assessment to determine the number of treatments required, which depends on the severity of infection and number of toes infected
·Photographs of nails before and after treatment
·Agree post-laser care programme
Is it painful?
There is no pain associated with the procedure, largely due to the lower heat Noveon® generates. There is no need to feel anxious – you are in good trained hands at Betafeet Podiatry!
What does it cost?
Betafeet Podiatry currently charges £600 for the whole cycle of treatment (reduced to £400 for a limited time.
What is the success rate?
Based on research, around 95 percent.
More information
See our Treatments and Services section on the home page: http://www.betafeetpodiatry.co.uk/fungal-nail-treatment which features a video interview with Judith Sullivan, Practice Owner/Manager.
Book now to take advantage of our special offer. We look forward to helping you get your toenails back in view this summer!