04 April 2016
Author/blogger Reggie Simpson
Support to help manage diabetes with confidence and control
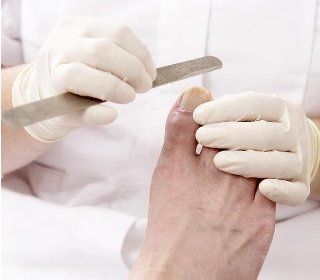
According to Diabetes UK, people with diabetes are at much greater risk of developing problems with their feet, due to the damage raised blood sugars can cause to sensation and circulation. If left untreated, these problems can cause foot ulcers and infections and, at worst, may lead to amputations. However, most foot problems are preventable with good, regular foot care.
Diabetes UK has an excellent guide to how to live with diabetes:
https://www.diabetes.org.uk/Guide-to-diabetes/Living_with_diabetes/
It is important for anyone who has diabetes to learn how to manage the condition. There are short courses, such as DAFNE (Dose Adjustment for Normal Eating) for Type I diabetes and DESMOND (Diabetes Education and Self Management for Ongoing and Newly Diagnosed) for Type II diabetes, which may help.
If you have diabetes and haven't yet attended an education programme, talk to your GP or diabetes care team as they can refer you to a local one. At Betafeet Podiatry we can also give you advice.
DAFNE is a way of managing Type 1 diabetes and provides people with the skills necessary to estimate the carbohydrates in each meal and to inject the right dose of insulin.
For more information visit the DAFNE website:
DESMOND (Diabetes and Self Management for Ongoing and Newly Diagnosed) is a UK NHS training course for those with Type II diabetes that helps people to identify their own health risks and to set their own goals.
For more information on DESMOND and diabetes care generally visit:
http://www.nhs.uk/Livewell/Diabetes/Pages/Healthfordiabetics.aspx
At Betafeet Podiatry, we aim to conduct a half-yearly foot assessment for our diabetic patients. We try to time this around six months after the patient has visited with his or her diabetic nurse or care team, and we are happy to provide the patient with a copy of our assessment to share with their diabetic health care team. In turn, we would like as much as possible for our diabetic patients to provide us with information such as their most recent Hb1Ac level. HbA1C is a measure of your average blood glucose level over 3 months. It was originally measured in percentages, but now is measured in millimoles per mol (mmol/mol).
Don’t let diabetes rule your life and those around you – take charge!